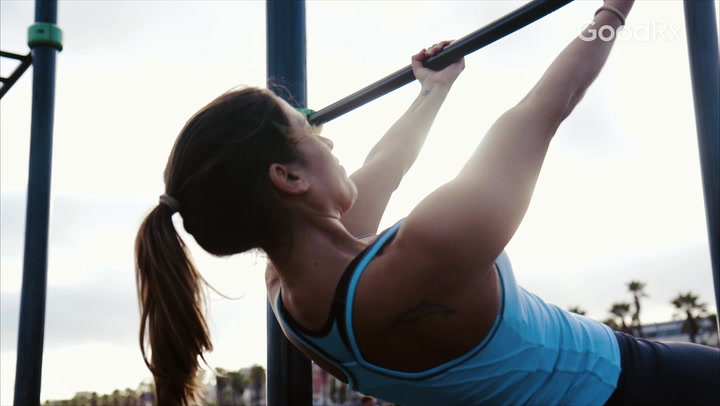Want to Avoid Osteoporosis Medications? Here Are Your Other Options
Key takeaways:
Osteoporosis medications improve bone strength and reduce the risk of hip and spine fractures.
Nonmedication treatments for osteoporosis include diet, exercise, and other lifestyle measures. Preventing falls (and fractures) is also very important.
In most cases, the benefits of taking an osteoporosis medication outweigh the risk of serious side effects.
Table of contents

Most people have no symptoms of osteoporosis, or weakening of the bones, until they break a bone. Fractures (breaks) due to osteoporosis can have serious long-term health consequences. If you have osteoporosis, it’s important to understand the risks and benefits of osteoporosis medications.
Let’s review the evidence behind medications for osteoporosis, as well as other treatments. This can guide you on choosing the best and safest treatment plan for osteoporosis.
How is osteoporosis treated?
Osteoporosis is usually treated with a combination of medication and lifestyle strategies.
There are several types of osteoporosis medications. The most common osteoporosis medications include:
Bisphosphonates: Bisphosphonates are usually the first-choice medication for treating osteoporosis.They work by preventing bone breakdown. Bisphosphonates like alendronate and risedronate are pills that are taken daily or once per week. Zoledronic acid is a bisphosphonate that’s given intravenously once a year.
Monoclonal antibodies: Denosumab (Prolia) treats osteoporosis by decreasing bone turnover. It’s given by injection every 6 months. Romosozumab (Evenity) works by increasing bone formation and reducing bone loss. It’s given as a monthly injection. Monoclonal antibodies are treatment options for people who aren’t improving on bisphosphonates or who are at very high risk for fracture.
Parathyroid hormone analogues: These medications act like parathyroid hormone in the body. They encourage bone growth, which helps to improve bone density. Osteoporosis medications like teriparatide and abaloparatide are good choices for people with very high risk for fracture.
People with osteoporosis can also improve bone health through lifestyle measures like:
Diet: Calcium and vitamin D are important for forming healthy bones. People with osteoporosis should make sure to get enough calcium and vitamin D either through diet or supplements.
Exercise: Weight-bearing exercise and strength training put stress on the bones and help improve bone density.
Avoiding or quitting smoking: Smoking contributes to bone loss. Research suggests that quitting smoking can improve bone health.
Avoiding heavy alcohol use: People with long-term, heavy alcohol use are at higher risk for osteoporosis.
How long do you have to take medication for osteoporosis?
It depends on the medication and your overall risk of fracture. Your healthcare professional can estimate your individual risk for fracture to help guide your decision.
If you have a low or moderate risk for fracture, your healthcare professional will likely recommend taking a bisphosphonate for 3 to 5 years. After that, they may recommend taking a break from the medication, called a medication holiday. This can reduce the risk of side effects from osteoporosis medications. There’s still some debate about how long a bisphosphonate holiday should last, and who should restart the medication after the holiday.
If you’re taking a monoclonal antibody or parathyroid hormone analogue for osteoporosis, the situation is a little bit different. These osteoporosis medications are more effective at building bone strength but have a greater risk of side effects.
Once you stop taking these medications, you’re more likely to have a rapid decrease in bone strength. That’s why people at very high risk for fracture often start off by taking denosumab or teriparatide then later switch to taking a bisphosphonate. This strategy helps build bone strength. It also reduces the risk of bone loss after stopping the first medication.
Which osteoporosis medication is best for me? From oral to injectable options, learn how to choose the best osteoporosis medication for you.
Exercise and bone strength: Resistance exercise can help your bone density. Learn more about exercising with osteoporosis.
Diet and bone health: What you need to know about eating for bone health.
Why don’t some people want to take osteoporosis medication?
There are several reasons why a person may hesitate to take medication for osteoporosis. Many people question why they should take medication to treat a condition that isn’t causing them any symptoms or problems right now. Other factors related to the medication might also contribute.
Side effects
As with any medication, side effects are possible with osteoporosis medications. Common ones include joint pain, nausea, and heartburn. Serious side effects like osteonecrosis of the jaw are possible, but they are rare.
The takeaway is this: If you have osteoporosis, your risk of breaking a bone is likely higher than your risk of serious side effects from treatment.
Pill burden
It can be frustrating to be given a new prescription to fill every time you see a healthcare professional. This is true especially if the medication doesn’t change how you feel or if you struggle with daily dosing. Some osteoporosis medications have strict requirements like remaining upright after you take them. These factors can make people not want to take the medication as prescribed.
Cost
New prescriptions can be costly. Ultimately, your insurance plan determines what your out-of-pocket cost for a new medication will be. In general, bisphosphonates are cheaper than other osteoporosis medications. Newer medications don’t have generic alternatives and may be more expensive. You can contact your insurance company directly to find out what your cost will be.
Taking time off for treatment
Unlike pills that you can take at home, some osteoporosis medications require a visit to a doctor’s office to be administered. But in most cases these treatments only need to be given once or twice a year. If time is a concern, talk with your healthcare professional about how often you’ll need treatment.
What can you do if you don’t want to take osteoporosis medication?
If you decide not to start medication for osteoporosis, there are things you can do to improve your bone strength. But keep in mind, while lifestyle measures can help, they’re not as effective as medications. For most people, lifestyle changes plus osteoporosis medication are the best strategy for preventing fractures due to osteoporosis.
Lifestyle strategies that can help reduce your risk from osteoporosis include:
Adjust your diet
A bone-healthy diet includes calcium and vitamin D. Adults generally need 1,000 mg to 1,200 mg of calcium daily. Good sources of calcium include milk and dairy products, green leafy vegetables, nuts, and calcium-fortified cereals. Limit cola sodas, which can lower your calcium levels. Vitamin D helps the body absorb calcium. You get vitamin D from sun exposure and foods like fatty fish and vitamin D-fortified cereal.
Avoid or quit smoking
People who smoke are more likely to get osteoporosis and break bones as they get older. Smoking affects the bones in a couple of ways. It makes it harder for the body to absorb calcium (which we need for strong bones), and directly affects the production of new bone. The good news is that bone health improves once you stop smoking.
Limit alcohol use
Heavy alcohol use increases the risk of osteoporotic fractures. Alcohol use can affect the bones by causing low calcium and vitamin D, affecting hormones that control bone strength, and interfering with the cells responsible for building bone. If you drink alcohol, you can reduce your risk for osteoporosis by drinking in moderation.
Prevent falls
It doesn’t take a big accident to break a bone if you have osteoporosis. Slipping and falling at home can be enough to break your wrist or hip. So it’s important to try to avoid falls. Follow these tips to make your home safer:
Make sure floors are clear. Remove clutter or objects that you can trip over, including rugs.
Keep your path well lit. Consider installing night lights to keep things bright when you need to get up at night.
Install handrails or grab bars. Make sure you can keep yourself balanced on stairs and in the bathroom.
Avoid slippery floors. Antislip mats can help prevent tile surfaces from becoming slippery when wet.
Wear shoes that fit. Avoid loose footwear or shoes with slick soles.
Build strength and balance
Exercise can help people with osteoporosis in a couple of different ways. Weight-bearing exercise and resistance training helps build bone strength. In addition, exercises that improve your balance can lower your risk of falls.
Talk with your healthcare professional before starting a new exercise program. For some people, working with a physical therapist is a good way to build strength and balance. Or you may try occupational therapy to learn how to more easily and safely go about your daily routine.
What happens if you don’t treat osteoporosis?
Without treatment, people with osteoporosis are at increased risk of fractures — especially of the vertebrae (spine), hip, and forearm (wrist). In fact, about half of all women and a quarter of all men will break a bone due to osteoporosis.
In older people, bone fractures can be very debilitating. Many people are not able to live independently after a hip fracture. In addition, a person’s risk of death increases after a hip fracture.
The most effective way to treat osteoporosis is a combination of lifestyle changes with medications. Treatment with bisphosphonates can reduce the chance of hip or spine fracture by 40% to 70% in some people with osteoporosis. So in many cases, taking osteoporosis medication is safer than going without treatment.
The bottom line
Treating osteoporosis with medication can significantly reduce the chances of hip or spine fracture. But if you decide to not take osteoporosis medication, there are other ways you can support bone health. These include eating a diet high in calcium and vitamin D, exercising to improve strength, and making changes at home to reduce your risk of falling. Speak with your healthcare professional to make sure you understand your personal risk for fracture to pick the best treatment plan for you.
References
Al-Bashaireh, A. M., et al. (2018). The effect of tobacco smoking on bone mass: An overview of pathophysiologic mechanisms. Journal of Osteoporosis.
Albrecht, B. M., et al. (2022). Adherence to lifestyle recommendations for bone health in older adults with and without osteoporosis: Cross-sectional results of the OUTDOOR ACTIVE study. Nutrients.
American Association of Clinical Endocrinology. (n.d.). All about osteoporosis.
Anupama, D. S., et al. (2023). Effect of lifestyle modification intervention programme on bone mineral density among postmenopausal women with osteoporosis. Sultan Qaboos University Medical Journal.
Ayers, C., et al. (2023). Effectiveness and safety of treatments to prevent fractures in people with low bone mass or primary osteoporosis: A living systematic review and network meta-analysis for the American College of Physicians. Annals of Internal Medicine.
Black, D. M., et al. (2020). Atypical femur fracture risk versus fragility fracture prevention with bisphosphonates. New England Journal of Medicine.
Brauer, C. A., et al. (2009). Incidence and mortality of hip fractures in the United States. JAMA.
Brown, J. P., et al. (2014). Bisphosphonates for treatment of osteoporosis: Expected benefits, potential harms, and drug holidays. Canadian Family Physician.
Callréus, M., et al. (2013). Adverse effects of smoking on peak bone mass may be attenuated by higher body mass index in young female smokers. Calcified Tissue International.
Chavda, S., et al. (2022). Osteoporosis screening and fracture risk assessment tool: Its scope and role in general clinical practice. Cureus.
Elbers, L. P. B., et al. (2021). Bone mineral density loss and fracture risk after discontinuation of anti-osteoporotic drug treatment: A narrative review. Drugs.
Godos, J., et al. (2022). Alcohol consumption, bone mineral density, and risk of osteoporotic fractures: A dose-response meta-analysis. International Journal of Environmental Research and Public Health.
Hanley, D. A., et al. (2012). Denosumab: Mechanism of action and clinical outcomes. International Journal of Clinical Practice.
Hayes, K. N., et al. (2021). Duration of bisphosphonate drug holidays in osteoporosis patients: A narrative review of the evidence and considerations for decision-making. Journal of Clinical Medicine.
Howland, R. H. (2009). Medication holidays. Journal of Psychosocial Nursing and Mental Health Services.
International Osteoporosis Foundation. (n.d.). Calcium recommendations.
Kiyota, Y., et al. (2020). Smoking cessation increases levels of osteocalcin and uncarboxylated osteocalcin in human sera. Scientific Reports.
Krupa, K., et al. (2023). Romosozumab. StatPearls.
Lin, K. (2023). ACP updates clinical recommendations on treatment of osteoporosis.
Morri, M., et al. (2019). One-year mortality after hip fracture surgery and prognostic factors: A prospective cohort study. Scientific Reports.
OrthoInfo. (n.d.). Smoking and musculoskeletal health.
Papaioannou, A., et al. (2007). Patient adherence to osteoporosis medications: Problems, consequences and management strategies. Drugs & Aging.
Rothem, D. E., et al. (2009). Nicotine modulates bone metabolism-associated gene expression in osteoblast cells. Journal of Bone and Mineral Metabolism.
Sampson, H. W. (1998). Alcohol’s harmful effects on bone. Alcohol Health and Research World.
Sampson, H. W. (2002). Alcohol and other factors affecting osteoporosis risk in women. Alcohol Research & Health.
Schnell, S., et al. (2010). The 1-year mortality of patients treated in a hip fracture program for elders. Geriatric Orthopaedic Surgery & Rehabilitation.
Sherrington, C., et al. (2020). Evidence on physical activity and falls prevention for people aged 65+ years: Systematic review to inform the WHO guidelines on physical activity and sedentary behaviour. International Journal of Behavioral Nutrition and Physical Activity.
Tucker, K. L., et al. (2006). Colas, but not other carbonated beverages, are associated with low bone mineral density in older women: The Framingham Osteoporosis Study. The American Journal of Clinical Nutrition.